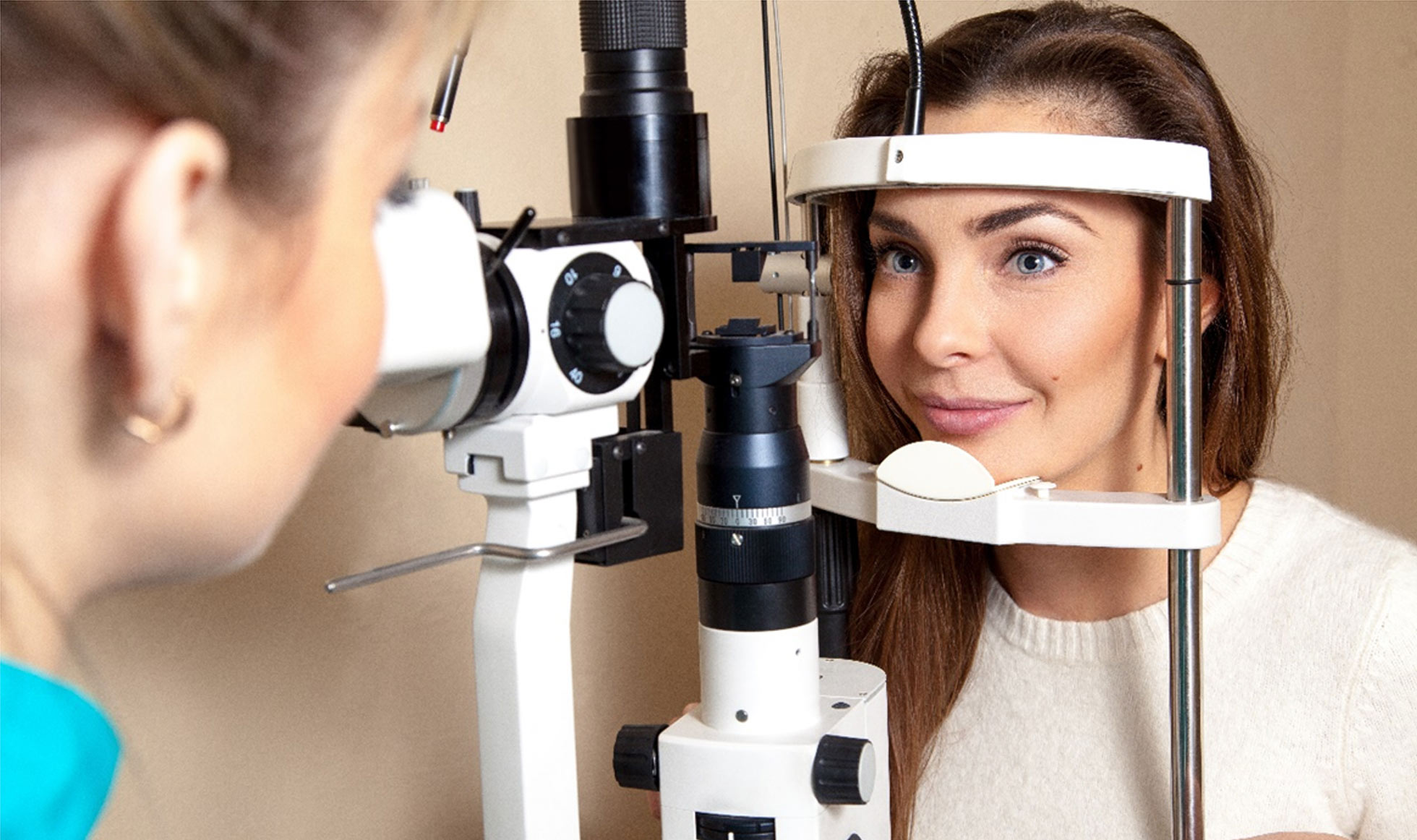
Anyone suspected of having a retinal artery occlusion should seek a same-day dilated examination with an ophthalmologist. During the exam, your vision will be measured, pupils dilated, and retinal images are taken. The eye doctor will examine your retinas and determine whether a blockage of blood flow has occurred. In most cases, the retina will appear pale where the loss of blood flow has caused swelling of the nerve fibers. Sometimes, the ophthalmologist can spot a particle of cholesterol within the retinal artery.
Sometimes a specialized imaging technique called fluorescein angiogram is helpful. During this test, dye is injected into an arm vein, and photos are taken as the dye passes through the retinal circulation. If an eye stroke has occurred, there will be a portion of the retina that does not light up with dye downstream of the blockage.
When retinal artery inflammation is suspected (temporal arteritis or giant cell arteritis), urgent lab testing is obtained. These tests (ESR and CRP) measure inflammation in the bloodstream. If these lab tests are elevated, the patient will be sent for a biopsy of the temporal artery for a definitive diagnosis of arterial inflammation.
If you experience a sudden loss of vision, seek an immediate dilated eye examination with a medical retina specialist. This exam may involve dilation, blood tests, photographs, or other specialized imaging tests of the retina.